Implant Treatments
Implant Treatments
Any artificial structure placed in the
human body is referred to as an implant. A dental implant is an artificial
tooth root made of titanium that is surgically placed into the jawbone in order
to restore the function and aesthetics of missing teeth. Titanium is a
biocompatible material that is well tolerated by the human body. Dental
implants have been used successfully since the 1960s, and with advances in
material and surface technologies, very high success rates are achieved today.
Tooth loss does not only cause
aesthetic problems but may also lead to impaired chewing function, digestive
issues, speech difficulties, and loss of self-confidence in social life.
Missing teeth can be restored using conventional methods such as fixed bridges
or removable dentures; however, in suitable cases, implant-supported prostheses
provide a highly effective treatment alternative. Implant therapy can be
planned for a wide range of clinical situations, from single tooth loss to
complete edentulism, provided that sufficient bone volume, good oral hygiene,
and an appropriate general health status are present.
Indications for Dental Implants
Single
or multiple tooth loss:
A single implant can be placed to
replace one missing tooth. In cases of multiple missing teeth, the number of
implants is determined based on the extent of tooth loss and the available bone
volume.
Complete
edentulism:
In
patients who cannot tolerate removable dentures or whose dentures lack adequate
retention, implants can be used to support prosthetic rehabilitation.
·
With
2–4 implants, a removable denture with improved retention can be fabricated.
·
With
6–8 implants, a fixed implant-supported prosthesis can be provided without the
need for a removable denture.
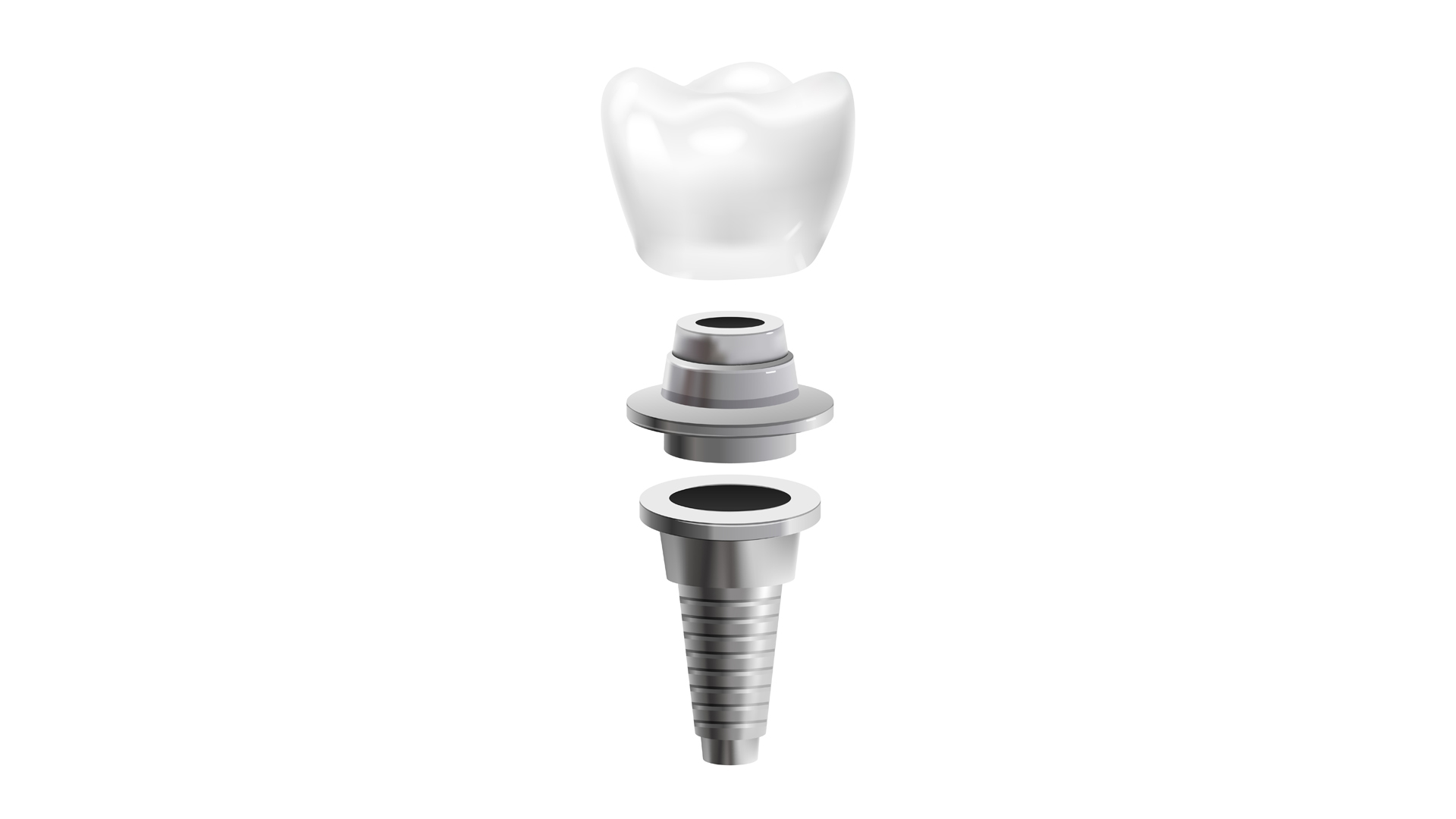
Structure of Dental Implants
Dental implants are manufactured from
titanium, a biocompatible and durable material. Titanium has a very low risk of
allergic reaction and integrates with the surrounding bone through a biological
process known as osseointegration, which allows the implant to become firmly
anchored in the jawbone.
Stages of Implant Treatment
Before treatment, the dentist performs
a thorough clinical and radiographic evaluation. Bone height and width, nerve
and sinus anatomy, gingival health, and the patient’s systemic health status
are assessed. When necessary, three-dimensional imaging (CBCT) and blood tests
may be requested. After explaining the treatment plan and prosthetic options in
detail, informed consent is obtained.
The surgical procedure is performed
under local anesthesia. The gingiva is opened, a socket is prepared in the
bone, and the implant is placed into the prepared site. The area is then
sutured. No pain is felt during the procedure; mild swelling and discomfort
after surgery are usually temporary and can be managed easily. A healing period
of approximately 3–6 months is generally required for osseointegration.
Temporary prostheses may be used during this period. In selected cases with
sufficient primary stability, prosthetic rehabilitation may be initiated earlier
using modern implant systems.
Anatomical structures such as the
maxillary sinuses in the upper jaw or the mandibular canal in the lower jaw, as
well as insufficient bone volume, may limit implant placement. In such cases,
bone augmentation procedures (bone grafting, sinus lift, etc.) may be performed
either simultaneously or in a separate session, which may extend the overall
treatment duration.
Postoperative Care and Follow-Up
Meticulous oral hygiene and regular
dental follow-up appointments are essential for long-term implant success. Poor
oral hygiene, smoking, and excessive alcohol consumption significantly increase
the risk of peri-implant inflammation. Adherence to the dentist’s instructions
and regular check-ups help prolong the lifespan of the implants.
Is Dental Implant Treatment Suitable for Everyone?
In young individuals, implant placement
is only recommended after completion of skeletal growth (approximately 16–17
years in females and 18 years in males). There is no upper age limit in adults;
implants can be placed in any patient with adequate bone structure and suitable
general health.
Can Dental Implants Be Rejected by the Body?
Dental implants are made of titanium
and are not rejected by the immune system. However, in rare cases, implant failure
may occur due to infection, insufficient bone support, or inadequate oral
hygiene. This situation is not considered a “rejection” but rather a biological
or mechanical complication.
Contraindications for Implant Treatment
Implant
therapy may be postponed or contraindicated in cases such as:
· Uncontrolled
systemic diseases
·
Poorly
controlled diabetes mellitus
·
Insufficient
bone volume that cannot be surgically augmented
·
Patients
unable to maintain adequate oral hygiene
Factors Affecting Implant Success
Implant
success is directly related to:
·
the
patient’s general health status,
·
bone
quality and volume,
·
smoking
and alcohol consumption,
·
oral
hygiene habits,
·
regular
maintenance and follow-up.
As
long as the surrounding bone and soft tissues remain healthy, dental implants
can be used safely and effectively for many years.
- Veneer & Smile Design: Enhancing Your Smile with Precision
- Emax Crowns: A Guide to the Latest Dental Technology
- Zirconium Crowns
- Digital Smile Design: Enhancing Your Smile with Technology
- Hollywood Smile
- Tooth Diamond, Tattoo, and Dental Grillz: A Professional Guide
- Implant Treatments
- General Anaesthesia: A Professional Overview
- All-on-4 vs All-on-6 Implant Treatment Options: Which is Right for You?
- Jaw Tumor and Fracture: A Professional Overview
- Snoring Treatment
- Temporomandibular Joint Issues
- Surgical Procedures
- Bad Breath Treatment: Effective Solutions for Fresher Breath
- Dental Spa: A Professional Approach to Oral Health
- Teeth Grinding: Causes, Symptoms, and Treatment
- Periodontology (Gum) Treatments
- Gum Aesthetics – Pink Aesthetic
- Restorative Dentistry
- Inlay-Onlay Fillings: A Professional Guide
- Sensitive Dental Treatment: Tips for Managing Pain During Procedures
- Orthodontic Treatment
- Clear Aligners (Invisalign): The Transparent Alternative to Traditional Braces
- Endodontics: What You Need to Know About Root Canal Treatment
- Pedodontics (Pediatric Dentistry)
- Prosthetic Treatments in Dentistry: A Comprehensive Overview
- Teeth Whitening
