Endodontics: What You Need to Know About Root Canal Treatment
Endodontics: What You Need to Know About Root Canal Treatment
Pain
that develops in teeth with extensive caries or large restorations may be
intermittent in the early stages. Over time, however, it often becomes
persistent, sharp, and throbbing. In some cases, the pain is not limited to a
single tooth but may be felt throughout the entire affected region.
In
certain situations, patients may experience no pain at all, and a chronic
abscess is detected incidentally during routine radiographic examination. For
this reason, regular dental check-ups are of great importance.
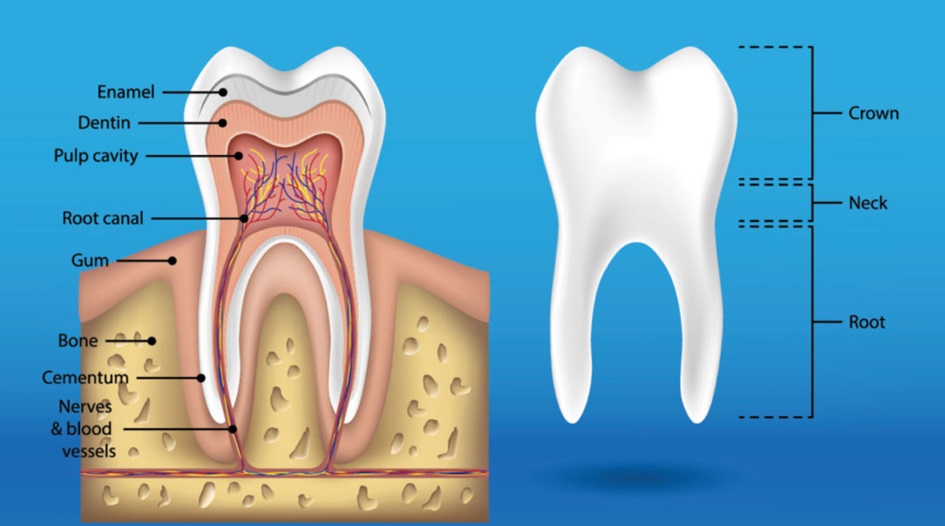
What Is the Pulp (Dental Nerve)?
The pulp is a soft tissue located
inside the tooth, containing nerves, blood vessels, and lymphatic tissue. It is
found within the narrow, tube-like root canals of the tooth root and within the
pulp chamber of the tooth crown.
The pulp is responsible for maintaining
the vitality of the tooth. However, once it becomes infected or irreversibly
damaged, it is unable to regenerate.
How
Does Dental Caries Progress?
If left untreated, dental caries
gradually deepens and damages the hard dental tissues and the pulp:
A: White
spot lesion (initial stage)
B: Progression into the enamel
C: Involvement of the dentin
D: Involvement of the pulp
E: Extension into the pulp with infection
Outcome: Abscess formation in the jawbone
When
caries is treated at an early stage, the problem can be resolved with a small
restoration. If progression is allowed, root canal treatment becomes
unavoidable.
Pulp Infection and Abscess Formation
When the pulp becomes diseased or
injured and fails to heal, it becomes infected. Untreated pulp tissue eventually
necroses, and the resulting inflammatory exudate (pus) accumulates at the root
apex. This may lead to resorption of the surrounding bone and the formation of
a periapical abscess.
Endodontic (root canal) treatment
initiates the body’s natural healing process by removing the infected pulp
tissue.
How Is Root Canal Treatment Performed?
With
current techniques, root canal treatment is planned to be completed in as few
appointments as possible in most cases.
Treatment
Steps:
·
Local
anesthesia is administered; the procedure is painless.
·
An
access cavity is prepared through the occlusal surface to reach the pulp
chamber.
·
The
infected pulp tissue is removed.
·
The
root canals are cleaned, shaped, and prepared for obturation.
·
If
treatment requires more than one visit, a temporary restoration is placed
between appointments.
During
this period, mild sensitivity or discomfort may be experienced.
·
At
the final appointment, the temporary restoration is removed, and the canals are
densely and hermetically filled.
·
After
completion of treatment, the tooth must be definitively restored.
Restoration After Root Canal Treatment
Depending on the amount of remaining
tooth structure, a direct restoration (filling) or a crown may be indicated.
In some cases, placement of an
intracanal post may be required to reinforce the tooth.
Frequently Asked Questions
Can
a root canal–treated tooth develop caries again?
Yes,
it can.
Caries
formation is associated with bacterial plaque. If oral hygiene is inadequate
(insufficient tooth brushing and flossing), root canal–treated teeth may also
develop caries. However, because these teeth are non-vital, caries-related pain
is usually not perceived and is often detected only during radiographic
examination.
Is
a root canal–treated tooth more prone to fracture?
Teeth
that have undergone root canal treatment typically have significant loss of
tooth structure and are therefore at increased risk of fracture. The most
effective way to reduce this risk is the placement of a full-coverage crown.
Does
a root canal–treated tooth continue to function normally?
Yes.
Although
the pulp tissue responsible for tooth vitality is removed, the surrounding bone
and gingival tissues remain vital. These tissues allow the tooth to continue
performing its normal masticatory function within the oral cavity.
- Veneer & Smile Design: Enhancing Your Smile with Precision
- Emax Crowns: A Guide to the Latest Dental Technology
- Zirconium Crowns
- Digital Smile Design: Enhancing Your Smile with Technology
- Hollywood Smile
- Tooth Diamond, Tattoo, and Dental Grillz: A Professional Guide
- Implant Treatments
- General Anaesthesia: A Professional Overview
- All-on-4 vs All-on-6 Implant Treatment Options: Which is Right for You?
- Jaw Tumor and Fracture: A Professional Overview
- Snoring Treatment
- Temporomandibular Joint Issues
- Surgical Procedures
- Bad Breath Treatment: Effective Solutions for Fresher Breath
- Dental Spa: A Professional Approach to Oral Health
- Teeth Grinding: Causes, Symptoms, and Treatment
- Periodontology (Gum) Treatments
- Gum Aesthetics – Pink Aesthetic
- Restorative Dentistry
- Inlay-Onlay Fillings: A Professional Guide
- Sensitive Dental Treatment: Tips for Managing Pain During Procedures
- Orthodontic Treatment
- Clear Aligners (Invisalign): The Transparent Alternative to Traditional Braces
- Endodontics: What You Need to Know About Root Canal Treatment
- Pedodontics (Pediatric Dentistry)
- Prosthetic Treatments in Dentistry: A Comprehensive Overview
- Teeth Whitening
